 
“I remember vividly believing I was in purgatory. At Northwestern Memorial Hospital, he was put on a ventilator twice in the ICU, for a total of nearly two weeks, and remembers having “a lot of hallucinations” - a symptom of delirium. 
Gordon Quinn, 77, a Chicago documentary filmmaker, believes he contracted Covid-19 at a conference in Australia in early March. Babar Khan, associate director of Indiana University’s Center for Aging Research at the Regenstrief Institute, and one of Walters’ physicians. “What we’re seeing with Covid-19 and older adults are rates of delirium in the 70% to 80% range,” said Dr. Wash your hands: Why this year's Global Handwashing Day is more important now than ever 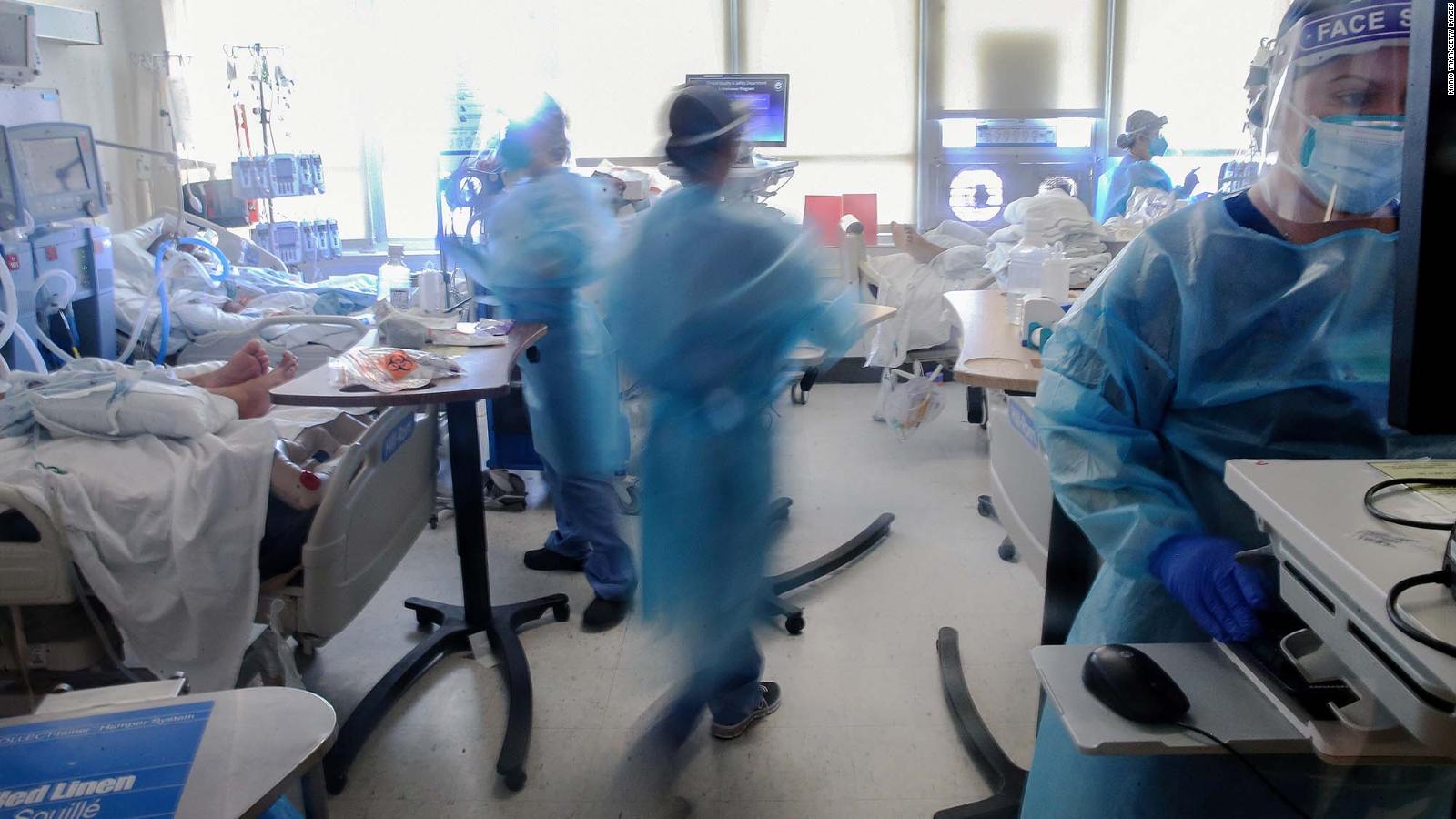
It can manifest as acute confusion and agitation or as uncharacteristic unresponsiveness and lethargy. In older adults, delirium is associated with a heightened risk of losing independence, developing dementia and dying. Seniors hospitalized for serious illness are susceptible to the often-unrecognized condition when they’re immobilized for a long time, isolated from family and friends, and given sedatives to ease agitation or narcotics for pain, among other contributing factors. The aftereffects of delirium - an acute, sudden change of consciousness and mental acuity - can complicate recovery from Covid-19. Most likely, he speculated, a year after fighting the disease at least half of the critically ill older patients will not be fully recovered. Wesley Ely, co-director of the Critical Illness, Brain Dysfunction and Survivorship Center at Vanderbilt University Medical Center. “Recovery will be on the order of months and years, not days or weeks,” said Dr. Younger adults who’ve survived a serious course of Covid-19 experience similar issues but older adults tend to have “more severe symptoms, and more limitations in terms of what they can do,” Chen said. I’ve been really nervous and jittery,” Walters said. “Emotionally, it’s been hard because I’ve always been able to do for myself, and I can’t do that as I like. I've been really nervous and jittery," she said. She calls it "brain fog." "Emotionally, it's been hard because I've always been able to do for myself, and I can't do that as I like. If I’m walking sometimes my legs get wobbly and my arms get like jelly.”Īs she recovers from Covid-19, Marilyn Walters finds it difficult to put thoughts together and remember recent events. Today, she said, “I still get tired real easy and I can’t breathe sometimes. Walters, who lives in Indianapolis, spent almost three weeks in March and April heavily sedated, on a ventilator, fighting for her life in intensive care. (Because of gaps in testing, the actual death rate may be lower.) Even among the age group at greatest risk - people 85 and older - just 28% of those with confirmed cases end up dying, according to data from the Centers for Disease Control and Prevention. Most seniors survive Covid-19 and will encounter these concerns to varying degrees. Other challenges abound: overcoming muscle and nerve damage, improving breathing, adapting to new impairments, regaining strength and stamina and coping with the emotional toll of unexpected illness. Photographer: Go Nakamura/Bloomberg via Getty Images Go Nakamura/Bloomberg/Getty ImagesĬhronic fatigue syndrome a possible long-term effect of Covid-19, experts say Covid-19 cases and hospitalizations have spiked since Texas reopened eight weeks ago, pushing intensive-care wards to full capacity and sparking concerns about a surge in fatalities as the contagion spreads. A nurse wearing protective gear treats a patient in the Covid-19 intensive care unit (ICU) at the United Memorial Medical Center (UMMC) in Houston, Texas, U.S., on Monday, June 29, 2020. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
